Boy scouts serving as messengers delivering food and some supplies to the homes of flu sufferers during
the pandemic. (Left Photo Above)
Source: http://christchurchcitylibraries.com/Heritage/Photos/Disc2/IMG0048.asp
A group of nurses who served during the epidemic. (Right Photo Above) Source: Google Images
the pandemic. (Left Photo Above)
Source: http://christchurchcitylibraries.com/Heritage/Photos/Disc2/IMG0048.asp
A group of nurses who served during the epidemic. (Right Photo Above) Source: Google Images
(Shortage of medical staff remaining): There was a large shortage of medical facilities or supplies and medical assistance in duration of the epidemic. With the increasing demand in medical facilities and supplies as the death toll mounted, there were never enough abled medical staff to nurse the amount of severely sick patients in the crisis situation. The crisis had taken its toll on the remaining medical staff because doctors and nurses around the country worked long hours tirelessly. Nurses remaining in New Zealand mostly worked 17 hours a day during the crisis. Despite continuously working under strenuous conditions by being surrounded with sick people and still being aware of the rapid and sudden spread of the virus from one person to another (even with little contact) medical workers forced themselves to overwork in order to treat as many patients as they possible could. Hence, medical workforces were considered as heroes. This shortage in the availability of medical workforce during the crisis was due to a large number of New Zealand medics being yet to return from military postings from the war. As a result, this forced the remaining medical staff in New Zealand to work even harder, exhausting themselves by rushing from one case to another, scribbling, prescriptions or calling ambulances and due to their constant exposure to people that were severely ill with the virus, many medical workers found themselves easily catching the flu and falling severely ill as well. Hence, with the increasing amount of medical assistance who stricken, there was an increase in the shortage of medical staff especially at the peak of the influenza pandemic when they were most needed. Many suburbs in Auckland were even left without a local GP. Furthermore, there was an insufficient number of nurses for the new wards as more nurses fell ill very suddenly. At one point, in Auckland Hospital, 140 out of 180 nurses came down with the flu. At Onehunga, all the local doctors were down and the third was left with an incredible amount of workload. On the 22nd of November, 82 of 116 nurses in Dunedin were down with the flu, four of whom had died. Also, 4 out of the 5 hospital surgeons had also caught the flu. As the condition of the flu among people became more and more severe this caused the medical supplies to run on a low. The combating of the pandemic was taken on at a smaller scale in smaller country towns with fewer medical resources and doctors as well as hospitals that were capable of dealing with major surgeries or diseases. Hence, these towns simply relied on a few available doctors and medical supplies.
(Volunteer medical workforce established): Large groups of medical workforces, made up of the remaining doctors, remaining nurses and sisters (especially the Sisters of Mercy) as well as volunteered medical workers, around New Zealand cities were put together to coordinate relief works and provide further medical assistance for flu sufferers; due to the rapid decline in remaining healthy doctors and nurses available in hospitals. The medical workforce was in charge of nursing the severe flu sufferers in hospitals and temporary emergency hospitals as well as providing medical assistance by travelling to the homes of people who were ill, in order to determine the severity of their case, give the patients’ medical advice or recommendations and to further nurse severe case. With the increase in flu sufferers especially in major cities such as Auckland and Wellington, it was difficult to coordinate medical relief organisations. This was because there were never enough medical workers available to keep up with the growing demands of medical assistance for severe cases in the crisis situation; which was calling for more urgency in medical workforce. However, similarly to other volunteer organisations, medical workers found themselves being exposed to the severe virus constantly. As a result, a large number of medical staff caught the flu and became severely ill. Some, even died. Despite the growth in the death toll from severe cases of influenza around New Zealand (as the flu had spread even further and quicker) the medical workforce continued to work tremendously hard to treat patients in serious conditions, hence putting their own selves at a much greater risk of falling ill or dying from succumbing the flu. They exhausted themselves by rushing from cases to cases. Relief workers also saw many horrific sights from severe sickness, to slum conditions, to poverty, to people living in misery. Relief workers avoided visitations to these places and only the volunteer nuns were brave enough to venture into these unhealthy conditions. In Dunedin, a newspaper correspondence had identified ‘slum areas’ in South Dunedin and the inner city. It was revealed that more than 843 houses were unconnected to sewage systems and relied on pit toilets. Health officials later suggested that the overcrowding in unhygienic conditions were large factors that had contributed to the rapid spread of the flu. As written in the ‘Black November’, “Volunteers rose to the occasion and likened their bravery to that of soldiers at the Front”. Many relief workers and ambulances had also made long journeys to rural townships to bring severely ill sufferers to the main hospitals in the cities. A Christchurch doctor, Henry Thacker who was an MP, had gone to Okains Bay and discovered nearly every household in the bay stricken with the flu and more cases were collected later. As a result, he organised an influenza ward, saving the lives of many because of his arrival and his establishment of the emergency centre. In smaller towns, the lack of availability in doctors had brought more people in communities to coordinate patrol systems and organise relief works together. As a result, some nurses were sent to bureaus to relieve in these towns and Maori communities. The Health Department had sent a nurse to relieve medically in the Maori settlement at Arowhenua.
(Hospitals and temporary hospitals):Furthermore, hospitals became filled with influenza cases very quickly. People were urged to only come to hospital if they had severe influenza cases and to make space for the rapidly increasing amount of severe influenza cases, other non urgent cased patients were sent homes to leave the hospital, urged not come to the hospital. This was intended for the hospital to have enough beds and doctors or nurses for severe influenza patients. At Auckland hospital, emergency accommodation was arranged for infectious cases such as the influenza at hand. However, as hospitals became full very quickly, medical relief organisations coordinated the establishments of emergency hospitals or emergency treatment centres wherever possible. Schools, churches, several large institutions and community halls were transformed into convalescent hospitals where beds were set up for the large numbers of severely ill patients to be treated or nursed in by a group of volunteer medical assistance. Places such as Kilbryde with 60 beds, Vermont Street Catholic Girls’ School with 150 beds and the boys’ school next door with 3 convalescent wards, St. Joseph’s School in Grey Lynn with 70 beds, as well as many other school halls were transformed into temporary hospitals for the crisis. Large parts of some hospitals were even converted to temporary influenza wards as the hospital itself were already filled with influenza cases, such as the Misericordia Hospital. In Wellington, these included places such as Mt. Cook Girls’ school and St. Patrick’s College. The Takapuna ship was transformed into a floating port temporary hospital. The Stuart Hall with 50 beds and Hanover Baptist Hall with 40 beds were transformed into temporary hospitals in Dunedin.
(Appeals for volunteers): From late October, newspaper notices began to fill with urgent appeals for more volunteers in relief organisations from the combat of the epidemic at hand. Most of these included appeals for more medical assistance in medical relief coordination. These newspaper appeals did manage to bring forth groups of volunteers. Many of which were school teachers, ex-nurses, shop assistance, librarians and typists. Amelia Bagley, who was in charge of nursing aid at the Health Department nursing aid in Auckland continued to appeal for more qualified nurses and other volunteers (especially younger women) who were able to volunteer in the duration of the pandemic, by placing advertisements on newspapers. District committees were also asked to refer all qualified nurses to Miss Bagley. Nurses were offered ten shillings a day, hence, encouraging more nurses to volunteers in the epidemic combat. In Christchurch, the hospital board paid a man to go around the city to chalk notices on the foot paths appealing for forty nurses. Despite a great response, not all volunteers were trained nurses. Hence, these volunteers had to simply be trained on the job, due to the desperation for more medical staff in the urgent situation. A handbill of basic nursing advice from the Health Department was handed to every household in rural communities and Maori settlements. However, as these had arrived only after the peak of the epidemic to Maori settlements, Maori communities were largely affected in the high death toll during the epidemic.
(Volunteer medical workforce established): Large groups of medical workforces, made up of the remaining doctors, remaining nurses and sisters (especially the Sisters of Mercy) as well as volunteered medical workers, around New Zealand cities were put together to coordinate relief works and provide further medical assistance for flu sufferers; due to the rapid decline in remaining healthy doctors and nurses available in hospitals. The medical workforce was in charge of nursing the severe flu sufferers in hospitals and temporary emergency hospitals as well as providing medical assistance by travelling to the homes of people who were ill, in order to determine the severity of their case, give the patients’ medical advice or recommendations and to further nurse severe case. With the increase in flu sufferers especially in major cities such as Auckland and Wellington, it was difficult to coordinate medical relief organisations. This was because there were never enough medical workers available to keep up with the growing demands of medical assistance for severe cases in the crisis situation; which was calling for more urgency in medical workforce. However, similarly to other volunteer organisations, medical workers found themselves being exposed to the severe virus constantly. As a result, a large number of medical staff caught the flu and became severely ill. Some, even died. Despite the growth in the death toll from severe cases of influenza around New Zealand (as the flu had spread even further and quicker) the medical workforce continued to work tremendously hard to treat patients in serious conditions, hence putting their own selves at a much greater risk of falling ill or dying from succumbing the flu. They exhausted themselves by rushing from cases to cases. Relief workers also saw many horrific sights from severe sickness, to slum conditions, to poverty, to people living in misery. Relief workers avoided visitations to these places and only the volunteer nuns were brave enough to venture into these unhealthy conditions. In Dunedin, a newspaper correspondence had identified ‘slum areas’ in South Dunedin and the inner city. It was revealed that more than 843 houses were unconnected to sewage systems and relied on pit toilets. Health officials later suggested that the overcrowding in unhygienic conditions were large factors that had contributed to the rapid spread of the flu. As written in the ‘Black November’, “Volunteers rose to the occasion and likened their bravery to that of soldiers at the Front”. Many relief workers and ambulances had also made long journeys to rural townships to bring severely ill sufferers to the main hospitals in the cities. A Christchurch doctor, Henry Thacker who was an MP, had gone to Okains Bay and discovered nearly every household in the bay stricken with the flu and more cases were collected later. As a result, he organised an influenza ward, saving the lives of many because of his arrival and his establishment of the emergency centre. In smaller towns, the lack of availability in doctors had brought more people in communities to coordinate patrol systems and organise relief works together. As a result, some nurses were sent to bureaus to relieve in these towns and Maori communities. The Health Department had sent a nurse to relieve medically in the Maori settlement at Arowhenua.
(Hospitals and temporary hospitals):Furthermore, hospitals became filled with influenza cases very quickly. People were urged to only come to hospital if they had severe influenza cases and to make space for the rapidly increasing amount of severe influenza cases, other non urgent cased patients were sent homes to leave the hospital, urged not come to the hospital. This was intended for the hospital to have enough beds and doctors or nurses for severe influenza patients. At Auckland hospital, emergency accommodation was arranged for infectious cases such as the influenza at hand. However, as hospitals became full very quickly, medical relief organisations coordinated the establishments of emergency hospitals or emergency treatment centres wherever possible. Schools, churches, several large institutions and community halls were transformed into convalescent hospitals where beds were set up for the large numbers of severely ill patients to be treated or nursed in by a group of volunteer medical assistance. Places such as Kilbryde with 60 beds, Vermont Street Catholic Girls’ School with 150 beds and the boys’ school next door with 3 convalescent wards, St. Joseph’s School in Grey Lynn with 70 beds, as well as many other school halls were transformed into temporary hospitals for the crisis. Large parts of some hospitals were even converted to temporary influenza wards as the hospital itself were already filled with influenza cases, such as the Misericordia Hospital. In Wellington, these included places such as Mt. Cook Girls’ school and St. Patrick’s College. The Takapuna ship was transformed into a floating port temporary hospital. The Stuart Hall with 50 beds and Hanover Baptist Hall with 40 beds were transformed into temporary hospitals in Dunedin.
(Appeals for volunteers): From late October, newspaper notices began to fill with urgent appeals for more volunteers in relief organisations from the combat of the epidemic at hand. Most of these included appeals for more medical assistance in medical relief coordination. These newspaper appeals did manage to bring forth groups of volunteers. Many of which were school teachers, ex-nurses, shop assistance, librarians and typists. Amelia Bagley, who was in charge of nursing aid at the Health Department nursing aid in Auckland continued to appeal for more qualified nurses and other volunteers (especially younger women) who were able to volunteer in the duration of the pandemic, by placing advertisements on newspapers. District committees were also asked to refer all qualified nurses to Miss Bagley. Nurses were offered ten shillings a day, hence, encouraging more nurses to volunteers in the epidemic combat. In Christchurch, the hospital board paid a man to go around the city to chalk notices on the foot paths appealing for forty nurses. Despite a great response, not all volunteers were trained nurses. Hence, these volunteers had to simply be trained on the job, due to the desperation for more medical staff in the urgent situation. A handbill of basic nursing advice from the Health Department was handed to every household in rural communities and Maori settlements. However, as these had arrived only after the peak of the epidemic to Maori settlements, Maori communities were largely affected in the high death toll during the epidemic.
Some people volunteered in the service of the washing linens from hospitals set up, during the epidemic.
(Left Photo Below) source: Google Images
(Left Photo Below) source: Google Images

(Driver volunteers): Many people had also volunteered in the ambulance services to transport medical supplies and medical assistance to the homes of flu sufferers. Due to the lack of available motor transportation to deliver medical assistance to check up on cases of influenza around New Zealand, many people had also volunteered to give their cars or other motor transportations for the use of being delivery cars for this purpose. Although the volunteering of motor vehicles for this purpose, had a slow response initially, more people offered their vehicles as the situation became more critical. The prominent people who offered their services, include Lawyers, accountants and businessmen. However, according to Geoffrey Rice, “The supply of drivers never quite matched the level of need…and not all (vehicles offered) were suitable for carrying very sick people.” The St. John Ambulance Association later reported that there were a total of about 500 volunteers constantly changing, 11000 visits made by medical workforces providing assistance for flu patients and 2000 patients transported. In Temuka, a 1916 Stubaker taxi became a familiar sight around the town, as it operated as an ambulance, ferrying patients to and from the temporary hospitals set up. Like many other vehicles that operated as ambulances, these were in demand during the crisis due to the urgency of the situation as the death toll continued to rise.
(Linen washers): With the increasing number of patients suffering from the influenza at the hospitals, there was a constant urgency for linens to be washed and cleaned to prevent the easy the spread of the virus from one patient to another, through the linens being infected with the disease from previous flu sufferers. There was a group of volunteers who would do this service of washing linens for hospitals. However, by volunteering during this pandemic crisis, this group of volunteers were constantly exposing themselves to the influenza virus. Therefore, they were constantly putting themselves at a much greater risk of contracting the severe flu, as did other groups of volunteers. Even so, volunteers all around New Zealand continued to work hard under the strenuous conditions with the severe virus prevailing, just to save the lives or relief the burden of flu sufferers during the crisis situation when people needed each other the most. Still, the demands for more volunteers during the pandemic continued to grow and increase with more and more severe influenza cases.
(Epidemic kitchens): Groups of volunteers were formed to provide medical relief or assistance for the stricken. Soup kitchens were established in which a large group of volunteers came together to cook hot soups for the large number (thousands) of flu sufferers. The delivery of these soups became very important in the survival of many flu sufferers as many people were laid down by the flu and were so sick that they were unable to even cook for themselves. By having hot soups, this meant that the patients did not have to rely on their own selves or stricken family members to feed themselves. Hence, this lifted a burden among severely sick people and the establishment of soup kitchens had allowed thousands of patients to have this necessary assistance of getting food to survive in this crisis situation, in a convenient way. The establishment of an efficient soup kitchen from the Women’s National Reserve during the month of November, were successful in providing more than 4000 people with food as the most critical point in the pandemic. These soups were mostly delivered to the flu sufferers by the citizens’ committee and the boy scouts who were volunteered as messengers delivering food and medical supplies to the door steps of patients who were down with the flu. Hence, boy scouts around the country were very much involved in relief efforts during the pandemic. Sisters at the Sacred Heart Convent in Wellington provided hot meals to feed relief workers at Wellington. Several large epidemic kitchens providing soup as well as food for stricken households who were laid down during the crisis were also established in Christchurch. These included the Women’s Reserve and Beath’s tearooms. Several schools also helped by setting up epidemic kitchens.
(Linen washers): With the increasing number of patients suffering from the influenza at the hospitals, there was a constant urgency for linens to be washed and cleaned to prevent the easy the spread of the virus from one patient to another, through the linens being infected with the disease from previous flu sufferers. There was a group of volunteers who would do this service of washing linens for hospitals. However, by volunteering during this pandemic crisis, this group of volunteers were constantly exposing themselves to the influenza virus. Therefore, they were constantly putting themselves at a much greater risk of contracting the severe flu, as did other groups of volunteers. Even so, volunteers all around New Zealand continued to work hard under the strenuous conditions with the severe virus prevailing, just to save the lives or relief the burden of flu sufferers during the crisis situation when people needed each other the most. Still, the demands for more volunteers during the pandemic continued to grow and increase with more and more severe influenza cases.
(Epidemic kitchens): Groups of volunteers were formed to provide medical relief or assistance for the stricken. Soup kitchens were established in which a large group of volunteers came together to cook hot soups for the large number (thousands) of flu sufferers. The delivery of these soups became very important in the survival of many flu sufferers as many people were laid down by the flu and were so sick that they were unable to even cook for themselves. By having hot soups, this meant that the patients did not have to rely on their own selves or stricken family members to feed themselves. Hence, this lifted a burden among severely sick people and the establishment of soup kitchens had allowed thousands of patients to have this necessary assistance of getting food to survive in this crisis situation, in a convenient way. The establishment of an efficient soup kitchen from the Women’s National Reserve during the month of November, were successful in providing more than 4000 people with food as the most critical point in the pandemic. These soups were mostly delivered to the flu sufferers by the citizens’ committee and the boy scouts who were volunteered as messengers delivering food and medical supplies to the door steps of patients who were down with the flu. Hence, boy scouts around the country were very much involved in relief efforts during the pandemic. Sisters at the Sacred Heart Convent in Wellington provided hot meals to feed relief workers at Wellington. Several large epidemic kitchens providing soup as well as food for stricken households who were laid down during the crisis were also established in Christchurch. These included the Women’s Reserve and Beath’s tearooms. Several schools also helped by setting up epidemic kitchens.
Kitchens, like the one in the photo above, were established; to feed the many volunteers and flu sufferers during the epidemic. (Left Photo Above)
Source: http://christchurchcitylibraries.com/Heritage/Photos/Disc2/IMG0053.asp
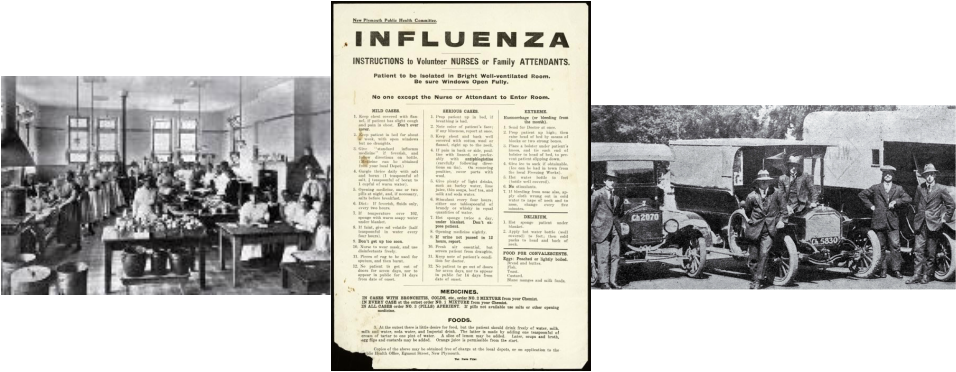
Influenza Nursing Instructions were handed to volunteer nurses or family members attending the sick during the epidemic; to educate them on how to deal with flu sufferers. (Middle photo Above)
Source: http://www.nzhistory.net.nz/media/photo/influenza-instructions-nurses
Members of the public had lend their vehicles for transportation purposes and many had also volunteered in ambulance services during the epidemic. (Right Photo Above) Source: Google Images
Source: http://christchurchcitylibraries.com/Heritage/Photos/Disc2/IMG0053.asp
Influenza Nursing Instructions were handed to volunteer nurses or family members attending the sick during the epidemic; to educate them on how to deal with flu sufferers. (Middle photo Above)
Source: http://www.nzhistory.net.nz/media/photo/influenza-instructions-nurses
Members of the public had lend their vehicles for transportation purposes and many had also volunteered in ambulance services during the epidemic. (Right Photo Above) Source: Google Images
The photo shows a large number of influenza epidemic ambulances parked outside the Wellington Town Hall during the epidemic (to provide medical relief for the large number of flu sufferers); some of which were private cars and commercial vans. (Left Photo Below) Source: http://www.nzhistory.net.nz/media/photo/wellington-ambulances-during-influenza-pandemic

(Workers and staff): In response to the rapid spread of the virus and the increasing number of sick people throughout New Zealand, many offices within companies had to close due to the lack of healthy staff members that were able to work. Public services were also halted or minimised and major factories were closed for the same reason. Furthermore, companies felt that if they were to continue working in the duration of the pandemic, the severity of the virus would have had major implications on other staff members and offices in which more workers would have been exposed to the flu or even overwork themselves if they were sick; when they needed to take a rest instead. Hence, this would have caused a loss in staff members in companies as workers could have fallen seriously ill or perhaps die, very quickly. Many companies, factories and services had made the decision to close to encourage the remaining abled staff members to volunteer in other services or organisations assisting in relief work during the crisis. Therefore, many companies in New Zealand took the approach and made the decision to stop the workload of staff members because they did not want to risk losing any more workers than they already have in this situation. They discouraged staff members from working to encourage the sick workers to take a rest while the remaining healthy staff could volunteer. In Wellington, larger firms such as ‘Kirkcaldie and Stains’ released hundreds of workers to nurse the sick and volunteer for relief work. As more and more people fell ill, they found it best to rest at home, hence changing the vibrant city of Auckland into an abnormal ‘City of Dead’ as described by Geoffrey Rice because the streets looked empty as people tried to avoid catching the flu by not travelling and working.
(Telephone exchange): Health Department offices and central bureaus were kept busy receiving and redirecting calls for assistance during the pandemic crisis. As a result, the telephone exchange and telephone lines were constantly flooded with calls directed to various places, which had led to a blockage in the phone lines. Hence, it was recommended for people to call for urgent medical assistance that were related to influenza only. Therefore, many people could not communicate to other family members during this time of crisis, when people needed the support of each other the most. With the workers working in hectic and stressful conditions, in was not surprising that the number of volunteers who became stricken with the flu, had increased rapidly during the crisis especially with overworking.
(Telephone exchange): Health Department offices and central bureaus were kept busy receiving and redirecting calls for assistance during the pandemic crisis. As a result, the telephone exchange and telephone lines were constantly flooded with calls directed to various places, which had led to a blockage in the phone lines. Hence, it was recommended for people to call for urgent medical assistance that were related to influenza only. Therefore, many people could not communicate to other family members during this time of crisis, when people needed the support of each other the most. With the workers working in hectic and stressful conditions, in was not surprising that the number of volunteers who became stricken with the flu, had increased rapidly during the crisis especially with overworking.
The photo below shows a group of volunteer nurses holding the babies who have been accommodated, in the duration of the epidemic, at the creches established during the pandemic. (Left Photo Below)
Source: http://www.teara.govt.nz/en/photograph/27790/children-affected-by-the-influenza-pandemic-1918
Source: http://www.teara.govt.nz/en/photograph/27790/children-affected-by-the-influenza-pandemic-1918

(Families): With whole families being stricken at the same time and having no one to assist or provide the necessities for the family, relief workers visiting the homes of flu sufferers reported many horrific conditions that people were living in. Due to the lack of a healthy person in many homes, people were living in insanitary and unhygienic conditions that were filled with severely sick and starving people. Newspapers printed these stories of sufferers living in poverty and slum like conditions around Auckland. For example, “A volunteer in Parnell found a house where a father, mother and nine children lay ill in two rooms, with a stick of furniture and four blankets between them all.”, as written in ‘Black November’. Healthy neighbours and other family members were the ones who usually took care of the children whose families or parents had been stricken with the flu. In rural townships, many farming’s had to come to a halt, with no available family members or neighbours being healthy enough to operate in farm work. Maori communities suffered huge losses in family members due the pandemic. Whina Cooper recalled; “Most of them, those I knew, they all died, and also the babies, they died… they had no place where they can be looked after, the only place that could be available, was Panguru school. They took all the patients there and just put them on the floor… All those people, there’s so many of them… Everyone was sick, no one to help they were dying one after the other…My father was very sick then. He was the first to die I couldn’t do anything for him. I remember we put him in a coffin, like a box. There were many others, you could see them on the roads, on sledges, the ones that are able to drag them away, dragged them to the cemetery. No time for tangis… it was a flu that was really eating you away… everybody looks weak and nobody wants to eat… I don’t think we had any medicine. But fumigating…”
(Crèche’s): As many young children were left unaware of the current crisis at hand, daycare centres were set up in which busy parents, or parents who were held up by many things during the crisis situation could leave their children in the day time. The YWCA and other crèche in Takapuna was set as accommodation for healthy young children to stay in for the duration of their parents being ill with the flu. For children who had caught the flu, temporary children’s influenza hospitals were also set up in Myers Kindergarten and at Ellerslie Racecourse. In Wellington, these included places such as the Miramar crèche and the Kelburn Centre. However, as with other temporary hospitals, the number of volunteered nurses never matched the level needed. In Dunedin, crèche’s were set up in the Presbyterian church on Maori Hill, the Anglican Boys’ home at Vauxhall and the Catholic orphanage in South Dunedin while in Christchurch, these were set up by the Plunket Society in Karitane Hospital in Cashmere for babies with stricken mothers, Bishopcourt in Park Terrace and in Mrs. F.H. Pyne’s house in Bealey Avenue. Sydenham Park was also used as a supervised playground with daytime activities and meals provided for children with deserving families, which was provided for more than 300 children daily.
(Crèche’s): As many young children were left unaware of the current crisis at hand, daycare centres were set up in which busy parents, or parents who were held up by many things during the crisis situation could leave their children in the day time. The YWCA and other crèche in Takapuna was set as accommodation for healthy young children to stay in for the duration of their parents being ill with the flu. For children who had caught the flu, temporary children’s influenza hospitals were also set up in Myers Kindergarten and at Ellerslie Racecourse. In Wellington, these included places such as the Miramar crèche and the Kelburn Centre. However, as with other temporary hospitals, the number of volunteered nurses never matched the level needed. In Dunedin, crèche’s were set up in the Presbyterian church on Maori Hill, the Anglican Boys’ home at Vauxhall and the Catholic orphanage in South Dunedin while in Christchurch, these were set up by the Plunket Society in Karitane Hospital in Cashmere for babies with stricken mothers, Bishopcourt in Park Terrace and in Mrs. F.H. Pyne’s house in Bealey Avenue. Sydenham Park was also used as a supervised playground with daytime activities and meals provided for children with deserving families, which was provided for more than 300 children daily.
(District committees and bureau’s set up): A central agency was set up; its purpose was to coordinate relief efforts and relief works around the city. In Auckland, the mayor, Sir James Gunson had decided to do so on the 31th of October. A citizens committee was established that included representatives of the Red Cross, St. John Ambulance Association, and a number of leading businessmen and trade union leaders. This group coordinated relief works for the pandemic crisis and responded to current situations during the pandemic in order to make major decisions or reestablishments for the next steps. Auckland city was divided into 22 districts; each having its own depot or bureau where residents were urged to apply or report for assistance, for serious cases. The establishments of blocks were also set up in other cities around New Zealand, hence giving each block the power to deal with the crisis situation in that district. Doctors were allocated to different blocks around cities so that there was a fair spread of doctors in towns and suburbs. Also, within each district bureau, the committees were given responsibility in coordinating and establishing relief works. Some relief measures in districts included house to house inspections. In Palmerston North, this included sanitary inspections, an issue of public notices, nursing advice and street disinfection. Throughout the month of November, newspapers were flooded with notices urging residents to report if there were serious cases in their households, to their respective borough councils or district committee. Many notices also appealed for volunteers to form borough councils or district committees. The central depot in Auckland was located at the Town Hall and it was originally intended to be ‘the clearing house’ for less than urgent requests for transport and medical supplies only. Also, the central depot held the main supply of medical provisions and equipment which were gain upon requests. However, due to the increasing number of severe flu patients, the central depot was easily swamped with urgent calls from the inner city (1900 in its first 5 days, 680 on 7th of November), leaving the other district committees to establish themselves, on their own. The citizens committee’s first act was to send an urgent appeal to Wellington for government assistance in combating the pandemic. The Minister of Health, however, had not realised the severity of the situation in Auckland and hence, did not take immediate action to combat the spread of the flu. His reply was largely criticised by the citizens committee as being “unsatisfactory” by Gunson, as if actions had been taken earlier, this could have changed and improved the outcome of the crisis situation. In Christchurch and Dunedin, the election of a central committee and the establishments of depots had already been taken into initiative before the other main cities in New Zealand. Nurse Maude was put in charge of the central bureau in Christchurch’s Cathedral Square, as elected by the Christchurch central committee. The greater preparation of the pandemic in these cities could have contributed to their greater outcome in the pandemic and greater organisations in further decisions or establishments regarding the crisis at hand.
(Doctors released from military postings and gazette was issued): The Health Department was urged to release doctors from military postings to medically assist the large number of flu sufferers. The District Health Officer, Dr. Frengley was also urged to visit Auckland immediately, to examine the situation. Frengley, as well as three army doctors, arrived in Auckland on the 3rd of November, and they were immediately send to relieve in areas where the doctors had been stricken. After examining the full extent of the situation in Auckland, Frengley was certain that from what he heard and saw, this was ‘no ordinary influenza’. The Minister of Health, Warren Russell had arrived in Auckland on the 5th of November and after some persuasion by Dr. Frengley to stay for 2 more days to visit district depots and inspect the overcrowded hospitals, Russell was convinced that a crisis or emergency situation was at hand and that New Zealanders were living in the midst or an existence of an epidemic. On Tuesday night, Russell issued a Gazette Extraordinary, declaring influenza a notifiable disease, which meant that local health authorities now had more power to combat this pandemic.
(Doctors released from military postings and gazette was issued): The Health Department was urged to release doctors from military postings to medically assist the large number of flu sufferers. The District Health Officer, Dr. Frengley was also urged to visit Auckland immediately, to examine the situation. Frengley, as well as three army doctors, arrived in Auckland on the 3rd of November, and they were immediately send to relieve in areas where the doctors had been stricken. After examining the full extent of the situation in Auckland, Frengley was certain that from what he heard and saw, this was ‘no ordinary influenza’. The Minister of Health, Warren Russell had arrived in Auckland on the 5th of November and after some persuasion by Dr. Frengley to stay for 2 more days to visit district depots and inspect the overcrowded hospitals, Russell was convinced that a crisis or emergency situation was at hand and that New Zealanders were living in the midst or an existence of an epidemic. On Tuesday night, Russell issued a Gazette Extraordinary, declaring influenza a notifiable disease, which meant that local health authorities now had more power to combat this pandemic.
A soldier is released, as shown in the photo, to assist the remaining volunteers in food distribution to flu sufferers during the epidemic. (Left Photo Above)
Source: http://christchurchcitylibraries.com/Heritage/Photos/Disc6/IMG0093.asp
The New Zealand Gazette Extraordinary was issued by Russell on the 13th of November 1918.
(Middle Photo Above) Source: Google Images
The photo shows the medicine department in Wellington's Central Bureau established during the pandemic; whereby the two women are bottling the standard influenza medication for distribution. (Right Photo Above) Source: Google Images
Source: http://christchurchcitylibraries.com/Heritage/Photos/Disc6/IMG0093.asp
The New Zealand Gazette Extraordinary was issued by Russell on the 13th of November 1918.
(Middle Photo Above) Source: Google Images
The photo shows the medicine department in Wellington's Central Bureau established during the pandemic; whereby the two women are bottling the standard influenza medication for distribution. (Right Photo Above) Source: Google Images
A volunteer holding the sign saying "All theatres closed until further notice" to warn the public that public places and facilities as such are closed in the duration of the pandemic. (Left Photo Below) Source: Google Images

(Public Transportation): As the timetables of public transportation were minimised, and in some districts, public transportation was halted, people could not travel to other areas of the city. It was made difficult for people to look after their friends who lived on the other side of the city due to the lack of public transportation available during the pandemic. People’s way of living had to also change to accommodate to the new rules on public transportation that were put in place. For many, this meant that they could not go to work (as some people still had to earn money) and hence, struggled to earn money in order to support the family during this crisis situation. However, the main purpose of minimising public transportation was due to the lack of healthy staff to operate the transportation and to also discourage people from travelling which could have assisted in the spreading of the viral disease as it gathered a large amount of people together. In Auckland, Dr Frengley ordered the railways and shipping companies to do “all within their power” to prevent any Maori from travelling in the duration of the epidemic. No Maori were given a ticket to travel on trains or ships without a signed permit from health authorities in Auckland. Hence, Maoris who were unable to travel on legitimate business as many were unable to get to Auckland to obtain the permit first. As a result, one woman whose son was dying, had been prevented to see him, like many other Maoris.
(Closure or public places): The government had ordered all public places where large groups of people would congregate or gather, to close in order to prevent further spread of the virus on the advice of medical experts. This included public halls, schools, hotels, theatres and places of entertainment such as billiard rooms and shooting galleries as with the rapid spread of the virus, the virus was able to spread from one person to another very quickly. Hence more people would be exposed to the virus and were very likely to catch the flu and fall very ill or die from just one person when gathered in large congregational areas. Public events and organisation meetings and race meetings were cancelled or postponed in the duration of the epidemic as ordered by Dr. Frengley. In Wellington, this meant that the Wanganui Agricultural Show and annual competitions were cancelled. However, the district health officers in Christchurch and Dunedin had already taken the initiative to do so, before official instructions from the Minister of Health. In the month of November, as the peak of the epidemic is reached, notices in that section of newspapers became prominently filled with notices in relation to the cancellation of meetings of certain groups. Churches were requested to hold services of a short duration and the Bishop of the Roman Catholic Church announced that all there would be no public services in Catholic Churches until the epidemic was over. With schools throughout the country ordered to close from the 7th of November until the New Year, schoolchildren were able to nurse their sick family members. Examination in schools were postponed and due to a death of a university student in Auckland, university examinations were also suspended. In Wellington, the official declaration for exams to be cancelled came on the 15th of November and students were sent home.The closure of hotel bars meant that alcohol stimulants could only be available by doctor’s prescription, at depots. The closure of all banks in New Zealand for a week to reduce the spread of the flu due to the gathering of people in banks, angered many New Zealanders as the public was greatly inconvenienced because no advance notice was given. Also, this caused a downfall in New Zealand’s commerce economy or market especially at a time when it was beginning to revive.
(Streets and portside disinfected and work halted): Streets and port sides or wharves were disinfected in an attempt to minimise the spread of the virus in the major streets and wharves around New Zealand as the increasing rapid spread of the flu was beginning to take its toll in certain areas, especially with more and more portside workers falling ill. In Wellington, wharves were sprayed twice daily with strong disinfectant. Further works was organised to combat the flu along waterfronts such as the establishments of more inhalation chambers for watersiders and seamen which opened on the 6th of November in Wellington. A recorded 45000 visitors had made use of this chamber. With the stopping of portside operations in Wellington, troopships and cruises such as the ‘Interislander’ and the ‘Maori’ that were due in Wellington could not dock in the Wellington harbour. The remaining ships at wharves were fumigated and cleaned from November 12th after the discovery of unhygienic conditions and overcrowding of severely sick people in ships upon inspections. As the severe virus continued to spread rapidly, the number of vessel crew member who were unavailable to work, continued to increase. As a result, coastal shipping especially in Wellington came to a standstill, with operations halted. The stopping of factory production and shipping in New Zealand had a negative effect on the delivery and production of sugar, coal and flour; which were largely needed and in huge demand for the epidemic crisis. With the food supplies running low, many shops and butchers struggled as these supplies easily ran out of the stocks or had only a few left, and the demands for these food supplies and more stocks for the crisis kept on increasing due to the crisis situation. Some temporary hospitals also relied on coal to heat their furnace. However, as the supplies for coal were running low, they easily ran out and temporary hospitals had to carry on in the demanding conditions. In Dunedin, the coaster ‘Calm’ were unable to unload a cargo of banana’s which were largely popular during the epidemic months, due to waterside operations halted. Hence, there was a large shortage in the stock for many fruits during the epidemic District Health officer in Christchurch, Dr. Chesson had ordered a general clean up and disinfection of the city. Also, he had asked the police to enforce the by-law against spitting in public.
(Closure or public places): The government had ordered all public places where large groups of people would congregate or gather, to close in order to prevent further spread of the virus on the advice of medical experts. This included public halls, schools, hotels, theatres and places of entertainment such as billiard rooms and shooting galleries as with the rapid spread of the virus, the virus was able to spread from one person to another very quickly. Hence more people would be exposed to the virus and were very likely to catch the flu and fall very ill or die from just one person when gathered in large congregational areas. Public events and organisation meetings and race meetings were cancelled or postponed in the duration of the epidemic as ordered by Dr. Frengley. In Wellington, this meant that the Wanganui Agricultural Show and annual competitions were cancelled. However, the district health officers in Christchurch and Dunedin had already taken the initiative to do so, before official instructions from the Minister of Health. In the month of November, as the peak of the epidemic is reached, notices in that section of newspapers became prominently filled with notices in relation to the cancellation of meetings of certain groups. Churches were requested to hold services of a short duration and the Bishop of the Roman Catholic Church announced that all there would be no public services in Catholic Churches until the epidemic was over. With schools throughout the country ordered to close from the 7th of November until the New Year, schoolchildren were able to nurse their sick family members. Examination in schools were postponed and due to a death of a university student in Auckland, university examinations were also suspended. In Wellington, the official declaration for exams to be cancelled came on the 15th of November and students were sent home.The closure of hotel bars meant that alcohol stimulants could only be available by doctor’s prescription, at depots. The closure of all banks in New Zealand for a week to reduce the spread of the flu due to the gathering of people in banks, angered many New Zealanders as the public was greatly inconvenienced because no advance notice was given. Also, this caused a downfall in New Zealand’s commerce economy or market especially at a time when it was beginning to revive.
(Streets and portside disinfected and work halted): Streets and port sides or wharves were disinfected in an attempt to minimise the spread of the virus in the major streets and wharves around New Zealand as the increasing rapid spread of the flu was beginning to take its toll in certain areas, especially with more and more portside workers falling ill. In Wellington, wharves were sprayed twice daily with strong disinfectant. Further works was organised to combat the flu along waterfronts such as the establishments of more inhalation chambers for watersiders and seamen which opened on the 6th of November in Wellington. A recorded 45000 visitors had made use of this chamber. With the stopping of portside operations in Wellington, troopships and cruises such as the ‘Interislander’ and the ‘Maori’ that were due in Wellington could not dock in the Wellington harbour. The remaining ships at wharves were fumigated and cleaned from November 12th after the discovery of unhygienic conditions and overcrowding of severely sick people in ships upon inspections. As the severe virus continued to spread rapidly, the number of vessel crew member who were unavailable to work, continued to increase. As a result, coastal shipping especially in Wellington came to a standstill, with operations halted. The stopping of factory production and shipping in New Zealand had a negative effect on the delivery and production of sugar, coal and flour; which were largely needed and in huge demand for the epidemic crisis. With the food supplies running low, many shops and butchers struggled as these supplies easily ran out of the stocks or had only a few left, and the demands for these food supplies and more stocks for the crisis kept on increasing due to the crisis situation. Some temporary hospitals also relied on coal to heat their furnace. However, as the supplies for coal were running low, they easily ran out and temporary hospitals had to carry on in the demanding conditions. In Dunedin, the coaster ‘Calm’ were unable to unload a cargo of banana’s which were largely popular during the epidemic months, due to waterside operations halted. Hence, there was a large shortage in the stock for many fruits during the epidemic District Health officer in Christchurch, Dr. Chesson had ordered a general clean up and disinfection of the city. Also, he had asked the police to enforce the by-law against spitting in public.
One of the 6 tram to have been converted into an inhalation chamber during the pandemic whereby members of the public can walk through it to be sprayed with zinc sulfate gas. (Left Photo Above)
Source: http://christchurchcitylibraries.com/Heritage/Photos/Disc6/IMG0094.asp
A bazaar stand to have been converted into a medicine depot, distributing the standard influenza medication, in one of the districts during the pandemic. (Middle Photo Above)
Source: http://www.nzhistory.net.nz/culture/influenza-pandemic-1918/influenza-depot
A woman is being sprayed, to her throat, by the gas mixture of Zinc Sulfate during the crisis (which had been a recommended precaution). Other members of the public are awaiting in a line for their turn to do so as well. (Right Photo Above)
Source: http://christchurchcitylibraries.com/Heritage/Photos/Disc18/IMG0052.asp
Source: http://christchurchcitylibraries.com/Heritage/Photos/Disc6/IMG0094.asp
A bazaar stand to have been converted into a medicine depot, distributing the standard influenza medication, in one of the districts during the pandemic. (Middle Photo Above)
Source: http://www.nzhistory.net.nz/culture/influenza-pandemic-1918/influenza-depot
A woman is being sprayed, to her throat, by the gas mixture of Zinc Sulfate during the crisis (which had been a recommended precaution). Other members of the public are awaiting in a line for their turn to do so as well. (Right Photo Above)
Source: http://christchurchcitylibraries.com/Heritage/Photos/Disc18/IMG0052.asp
(Methods and prevention and remedies): Many people tried different methods of preventing catching the flu. The most common of these was the use of inhalation stations, as recommended by the Health Department, in which people were able to go into rooms and have sprayers containing zinc sulphate which were sprayed down their throats. Further developments of this treatment led to the establishment of larger inhalation stations such as the inhalation chambers where large groups of people went into a room to breathe the sulphate gas. The first inhalation chambers in Auckland and Wellington were set up in the Town Halls while the Post Office building in Otago, became transformed into the first inhalation chamber there and it Christchurch, this had been the Electricity Department Building. Government employees were ordered to visit them daily and the number of public users for inhalation chambers continued to increase during the epidemic. It was also recommended for the public to go through these chambers before travelling to other parts of the country, whether by trains or ships. In Christchurch, 6 unused trams were converted into inhalation chambers in which compressed air braking units were installed to operate zinc sulphate sprayers. When people walked through these trams, the units would spray the zinc sulphate mixture in which they would breathe in this gas. The establishments of inhalation chambers around major areas and suburbs around New Zealand had been recommended by the Health Department as a method of precaution for the influenza virus. However, the success rates of this chambers and rooms were later questioned by the New Zealand public as having little or no effect and was medically useless in the prevention of catching the virus. In fact, it was later concluded that the use of inhalation chambers would have aided or assisted in the spreading of the flu as it gathered a large group of people to get sprayed together in one area. Hence, as people congregated to get sprayed, the virus could have easily spread from one person to another, rapidly. Therefore, it was only after the pandemic was over that people began to speculate the success of the inhalation chambers and proved that it had contributed to the increase in the spread of the flu. Many people had gone through inhalation chambers during the pandemic simply because it gave anxious people a reason to do something, that has been officially recommended, rather than just panic. Doctors were also sharply divided over the effectiveness of the sulphate sprays. Other remedies created to prevent succumbing the flu had included alcohol rubs, vitamins, baths, daily doses of quinine, and a teaspoon of sugar with a drop of kerosene. In many homes, a handful of sulphur was thrown into open fires in an attempt to fumigate the house. Lemon juice was another popular remedy and as a result, many shops ran out of lemons. However, these remedies were never proven conclusively to have a successful prevention rate for the influenza virus in the overall population. While some remedies could have actually had an effect to prevent catching the flu, many remedies could have been simply made allowing shop owners to make a larger profit during this time of struggle. These largely included fruit retailers in shops, that were still operating, that had continued to work in the epidemic duration, in which many were accused of raising prices fruits due to popular sales during the crisis. Many doctors had also experimented with different types of remedies to cure their flu patients. In Dunedin, Dr. Fitchett and Dr. Bowie, who took charge at the peak of the epidemic, tried aspirin, Eusol, bronchitis vaccine, mustard poultices, alcohol, morphine and heroin to ease the suffering of patients. Some doctors encouraged people to smoke to prevent catching the flu. Hence, many non-smokers were persuaded to take up smoking for the first time due to the pandemic prevailing.
(Medication and Standard medication by government): With the majority of flu sufferers resting at home, they were largely dependent on other family members to treat them and provide to their needs. However, as many flu sufferers were not visited by a medical staff, they were also largely reliant on patent influenza medication. These included popular brands such as Baxter’s Lung Preserver, Fluenzol (Bonnington’s Irish Moss) and Nazol and as the situation became more critical, more and more medication and disinfectant brands to prevent influenza, were advertised on the Newspapers such as Wawn’s Wonder Wool and U=Pino. As these products were in popular demand, this added to the burden for chemists and pharmacies to find enough stock especially at this situation when these products quickly ran out. Also, many businesses could not cope with the large amount of workload involved in dispensing or selling these products. As a result, many businesses were closed during the epidemic. This allowed the Health Department to devise a ‘Standard Influenza Remedy’ which was distributed to patients with a doctor’s prescription, at medicine depots which were located in the districts or blocks. Some bazaars or bazaar stands to raise fund for war efforts were converted into these medicine depots.
(Medication and Standard medication by government): With the majority of flu sufferers resting at home, they were largely dependent on other family members to treat them and provide to their needs. However, as many flu sufferers were not visited by a medical staff, they were also largely reliant on patent influenza medication. These included popular brands such as Baxter’s Lung Preserver, Fluenzol (Bonnington’s Irish Moss) and Nazol and as the situation became more critical, more and more medication and disinfectant brands to prevent influenza, were advertised on the Newspapers such as Wawn’s Wonder Wool and U=Pino. As these products were in popular demand, this added to the burden for chemists and pharmacies to find enough stock especially at this situation when these products quickly ran out. Also, many businesses could not cope with the large amount of workload involved in dispensing or selling these products. As a result, many businesses were closed during the epidemic. This allowed the Health Department to devise a ‘Standard Influenza Remedy’ which was distributed to patients with a doctor’s prescription, at medicine depots which were located in the districts or blocks. Some bazaars or bazaar stands to raise fund for war efforts were converted into these medicine depots.
A large crowd had gathered in Christchurch's Cathedral Square to celebrate the Armistice or 'end of war'. This largely contributed to the viral spread of the influenza virus. (Left Photo Below)
Source: http://www.nzhistory.net.nz/media/photo/armistice-day-celebrations-christchurch
Source: http://www.nzhistory.net.nz/media/photo/armistice-day-celebrations-christchurch

(Large gatherings and congregations): Despite early signs and warnings of the dangers of the influenza disease, many people were oblivious to the epidemic at hand and the existence of the severity of the flu. Hence, a large number of people gathered in large crowds to celebrate the end of war. In Auckland, a false notice of the armistice brought together a large crowd of people in Queen Street as well as other city hotels to celebrate the end of war. However, the congregation of lot of sick people meant that the severe virus was able to spread from one person to another rather quickly and within days, the number of people who were down with influenza had increased dramatically. Dr. Frengley blamed these celebrations as a contributing cause in the rapid spread of the flu and blamed people’s ignorance to the crisis situation for the increasing death tolls of influenza cased patients. Dr. Frengley banned any official celebrations for the real armistice during November, postponing celebrations for the war victory until the middle of 1919 for Auckland. However, in Christchurch, the Armistice celebration continued as planned which would have largely contributed to the increase in death toll, from influenza cases, in the following month. In Christchurch, it was the celebrations in the annual race carnival and agricultural show which had brought a large crowd of people together; many were also from the North Island (as the Health Department had failed to suspend the ferries from wellington to Lyttelton at this time) and many also came from locals in rural communities. This event had similar effects in the spreading of the severe virus rapidly from one person to another in the South Island, as compared to the Auckland Armistice celebration.
One of the many temporary hospitals set up during the epidemic, to accommodate the increasing number of severely ill flu sufferers. These became filled very quickly. (Left Photo Above) Source: Google Images
The urgent demands for more volunteer ambulance services continued to increase with the number of severe cases of influenza during the pandemic; as shown in the photo with the medics lifting the flu sufferer on a stretcher, into the ambulance van. (Middle Photo Above) Source: Google Images
Influenza depots were set up in districts to provide and supply the individual district with medical relief or assistance. (Right photo Above) Source: Google Images
The urgent demands for more volunteer ambulance services continued to increase with the number of severe cases of influenza during the pandemic; as shown in the photo with the medics lifting the flu sufferer on a stretcher, into the ambulance van. (Middle Photo Above) Source: Google Images
Influenza depots were set up in districts to provide and supply the individual district with medical relief or assistance. (Right photo Above) Source: Google Images
(Coffins and cemeteries): With the increasing number of deaths from cases of influenza around New Zealand there were too many bodies to provide proper burials for each individual victim. The thousands of coffins were made out of cheap timber. Hence, their lids were noticeably warped by sunshine. The coffins were also roughly made because the carpenters and joinery factories were in a hurry to get them done in order to keep up with the growing demand for more coffins as the death toll increased. As the urgency for the large number of bodies to be buried increased in Auckland, most bodies were carted in hundreds and these were sent to Victoria Park was used as the main temporary morgue. There, the bodies were laid out in orderly rows on the ground, wrapped up in canvas then placed under cover in the grandstand, awaiting to be transportation elsewhere for burial as the coffins could not be constructed quickly enough. In some areas, vans were required to collect the bodies in coffins for burials. In Onehunga, the mayor was seen with a horse and dray stacked with coffins. There were too many bodies for the volunteer coffin makers to keep up with and the demands kept on growing. However, no epidemic victims were cremated and all victims were placed into caskets for burials. The majority of bodies in Auckland were buried in Waikumete Cemetery, due to the large area that was able to be cleared to make space for the hundreds of bodies. This large space was dug by volunteers who worked tirelessly for long hours, to keep up with the demands to make space for more and more flu victims. Matthew Gray suggest that “People were terrified in those days because the flu was contagious so that they might even catch it from the dead bodies… the focus was on getting them underground as quickly as possible.” These caskets were stacked on special trains, which operated twice daily from November 13th to 20th of November, for transportation of these caskets to the cemetery for burial. Although most of the victims were buried without any headstones or mark of identification because “the speed involved there weren’t headstones placed on these graves.” as mentioned by Matthew Gray, complete records of victims that were buried at Waikumete Cemetery were kept. By the end of the epidemic, there were 444 burials at Waikumete, 210 at Waikaraka and 260 burials at Purewa. The remaining flu victims were buried at smaller cemeteries and churchyards. Wellington’s Karori cemetery recorded a total of 700 burials of influenza victims. In Christchurch, the main cemeteries for flu victims included the old Linwood cemetery and Bromley cemetery for the eastern side of the town as well as Sydenham and Addington cemeteries for the inner city victims. Large tents had been set up to accommodate the mourners and caskets of flu victims in these areas. Similar to situations elsewhere, with the increasing number of victims that were needed to be buried, the undertakers and grave diggers were forced to work long hours digging the space for burials as well as sorting out the identification of the flu victims that required burial. In Dunedin, most epidemic victims were buried at Andersons Bay cemetery and it was not uncommon to see a great number of funerals in the main street. Many people had had made extravagant funerals. For Maori communities, the Government had put a ban on tangis (funerals) during the pandemic crisis due to the negative perspectives, of Maori hygiene and sanitation, among the New Zealand Europeans. Therefore, with the Maori population generally regarded as dirty and filthy with editorials such as of ‘The Bay of Plenty Times’ printing Maoris as a “menace to health” from the customs such as tangis and The ‘Thames Star’ who referred to tangis as a “waste of time and substance of the Maoris and assist in the dissemination of disease.” With a ban on tangis and the insistence on prompt burials by the government, Maori flu victims were buried without the traditional ceremonies in shallow graves close to the temporary hospitals where they had died or schoolyards and church yards as well as marae’s. Hence, these places of burials were regarded as tapu (sacred) by Maori communities.
(Thanking): The end of the epidemic crisis marked an end of the sufferings and hardships throughout the country. For the people who had volunteered during the pandemic, their works were greatly appreciated by the Health Department and hospital boards throughout New Zealand. Hundreds of volunteers were formally thanked as they were rewarded with a certificate of appreciation from hospital boards and government. In Christchurch, volunteers were treated to a picnic in which cars were provided for 500 volunteers. Canon King, who was in charge of relief coordination in Dunedin, was regarded as Dunedin’s hero. He was presented with a cheque for 1000 pounds, a new motor car for his continuous social work and an award of recognition. 600 pounds was granted by the Christchurch City Council to Nurse Maude’s Nursing Association and Nurse Maude had her car hauled and repainted over by the expense of the AA. The Automotive Association in Christchurch were also formally thanked. The Minister of Health later paid a public tribute to the work of St. John Volunteers during the epidemic.
(Thanking): The end of the epidemic crisis marked an end of the sufferings and hardships throughout the country. For the people who had volunteered during the pandemic, their works were greatly appreciated by the Health Department and hospital boards throughout New Zealand. Hundreds of volunteers were formally thanked as they were rewarded with a certificate of appreciation from hospital boards and government. In Christchurch, volunteers were treated to a picnic in which cars were provided for 500 volunteers. Canon King, who was in charge of relief coordination in Dunedin, was regarded as Dunedin’s hero. He was presented with a cheque for 1000 pounds, a new motor car for his continuous social work and an award of recognition. 600 pounds was granted by the Christchurch City Council to Nurse Maude’s Nursing Association and Nurse Maude had her car hauled and repainted over by the expense of the AA. The Automotive Association in Christchurch were also formally thanked. The Minister of Health later paid a public tribute to the work of St. John Volunteers during the epidemic.
The memorial stone and the mass grave in Waikumete Cemetery where the thousands of influenza victims in Auckland were buried. (left Photo Above) Source: Google Images
The certificate of appreciation from the Health Department given to the Otago Hospital Board on behalf of all the volunteers who assisted in that district during the pandemic crisis. Other District Boards received a
similar certificate. (Middle photo Above) Source: Google Images
The grave of Private Thomas Graham (located at Waikumete Cemetery); he one of the many soldiers returning from war who had died from the influenza disease in New Zealand. (Right Photo above) Source: Google Images
The certificate of appreciation from the Health Department given to the Otago Hospital Board on behalf of all the volunteers who assisted in that district during the pandemic crisis. Other District Boards received a
similar certificate. (Middle photo Above) Source: Google Images
The grave of Private Thomas Graham (located at Waikumete Cemetery); he one of the many soldiers returning from war who had died from the influenza disease in New Zealand. (Right Photo above) Source: Google Images